The third permanent molar teeth are commonly known as wisdom teeth. They are found at the very back of the mouth in either the upper and/or lower jaws. They are often very troublesome for patients to keep clean. Generally, they begin to erupt between the ages of 17 and 26-years-old but patients can have problems with them at any stage of their lives from this point. The eruption of wisdom teeth occurs naturally and there are currently no means of controlling or alleviating this process. Some people are born without any wisdom teeth and are perceived as being “more evolved” – apparently as more babies now have shorter faces, smaller mouths and therefore reduced space for additional teeth. Another myth, is that wisdom teeth cause crowding of the lower incisors; however, there is no evidence of this and it’s thought the crowding is due to late growth from the lower jaw.
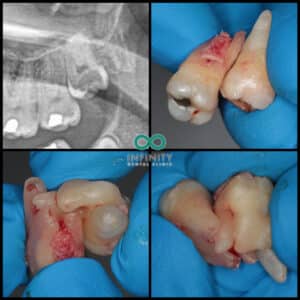
Around a quarter of wisdom teeth fail to erupt fully into the mouth or only erupt partially, however, patients can still get problems from them. Often wisdom teeth can also become impacted. Impaction is when a wisdom tooth cannot erupt into a normal and functional position (despite the tooth’s roots being completely formed) because it is stuck behind another tooth or covered by gum and/or bone. When any tooth is impacted it becomes much more difficult to keep clean and the risk associated with developing disease from it is much higher. There are various terms used to categorise impaction, some are included in the images of our patients’ teeth and labelled below:
1 – Vertical Impaction
2 – Mesio-angular Impaction
3 – Horizontal Impaction
4 – Disto-angular Impaction
WHY DO WE GET PROBLEMS FROM THEM?
As noted above, wisdom teeth can be notoriously difficult to clean. When wisdom teeth are impacted, unerupted or partially erupted, patients find it sometimes nigh-on impossible to keep clean. Bacteria can get caught in-between a lower wisdom tooth and the lower second permanent molar (often seen in cases with horizontally-impacted and mesio-angularly impacted teeth), leading to tooth decay of either tooth or devastatingly sometimes both. This frequently leads to removal of the wisdom tooth alongside treatment of the second permanent molar with a filling or root-canal treatment with a crown or even extraction.
In the image below, this patient came to see us as their lower left second permanent molar had become loose and painful. We found that the wisdom tooth was mesio-angularly impacted and had actually destroyed part of the root holding in the lower left second permanent molar. This led to an unresolvable infection, sadly leading to the surgical removal of both teeth through no fault of this patient.
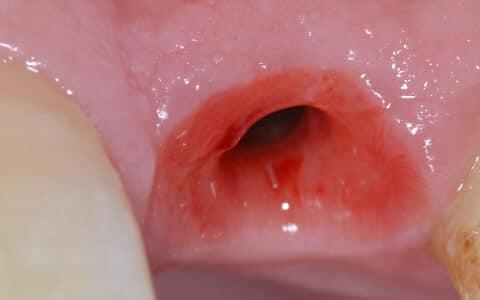
Patients can also develop problems from bacteria becoming trapped under the operculum (flap of gum overlying a partially erupted wisdom tooth), leading to signs and symptoms of pericoronitis which can include: pain, swelling, redness, bleeding, difficulty opening the mouth, bad breath, a foul taste and ultimately an infection.
Other problems can also include upper wisdom teeth over-erupting and traumatising the operculum of the lower wisdom tooth; or more rarely the formation of a cyst around the crown of an unerupted wisdom tooth. Usually, lower wisdom teeth are more challenging to remove than upper wisdom teeth, but there are rare occasions where the opposite is true.
In the image above, this patient had a partially erupted upper left wisdom tooth with a large cavity caused by tooth decay as she was physically unable to access and brush it, due to obstruction from the coronoid process (a segment of bone which is part of the lower jaw). This poor patient had the worst luck as we had to remove the functional upper left second permanent molar to be able to remove the wisdom tooth, as we noted that the wisdom tooth’s roots were locked into those of the upper left second permanent molar. Fortunately, our patient left happy having had these teeth removed as she’d had months of excruciating pain from a combination of tooth decay, bacteria stuck beneath the gum of the partially erupted tooth and because the tooth was trying to force itself out but its roots were stuck and locked into the roots of its neighbour. She was able to enjoy her holiday a few days later knowing we had resolved her pain and problems definitively.
HOW CAN THEY BE RESOLVED?
The issues above are conventionally resolved by removing the offending wisdom tooth. Antibiotics can be helpful as a short-term measure to alleviate an infection but more often than not, the problems will reoccur and removing the wisdom tooth is the only definitive solution. Cutting the flap of gum (operculectomy) where the tooth is partially erupted rarely helps as the gum usually just grows back.
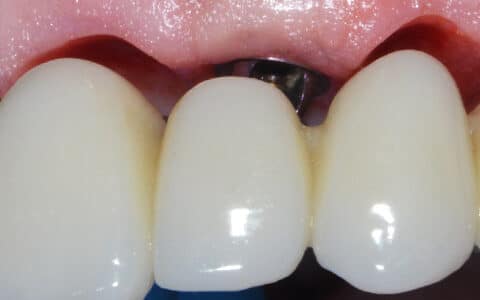
Here at Infinity Dental Clinic, we pride ourselves on expertise and providing the best quality of care for our patients. When patients attend our practice and we are considering the removal of a wisdom tooth, we would usually obtain an orthopantogram (OPT) image initially following their consultation. Appointments are then arranged to discuss the procedure required in more depth and this is tailored to each individual patient and their teeth – meaning our patients feel prepared before, during and after the procedure. Based on the assessment of the OPT, in some cases we will take a sectional cone-beam computed tomography (CBCT) scan to assess the tooth and surrounding anatomical structures further and discuss the findings. We are very fortunate to have a CBCT scanner in-house – most practices would need you to travel and attend elsewhere for this to be taken. Following this is the surgical removal of the wisdom tooth itself. In some rarer cases, we would undertake a coronectomy if there are concerns about a greater intimacy between the tooth’s roots in relation to the inferior alveolar (dental) nerve… But we’ll save that for another blog!
Ultimately, here at Infinity Dental Clinic, as well as creating beautiful smiles we also provide the highest quality dental healthcare to ensure our patients are happy from start to finish and receive the attention and care they deserve.
Thank you for taking the time to read this,
Dr Vinay Mistry